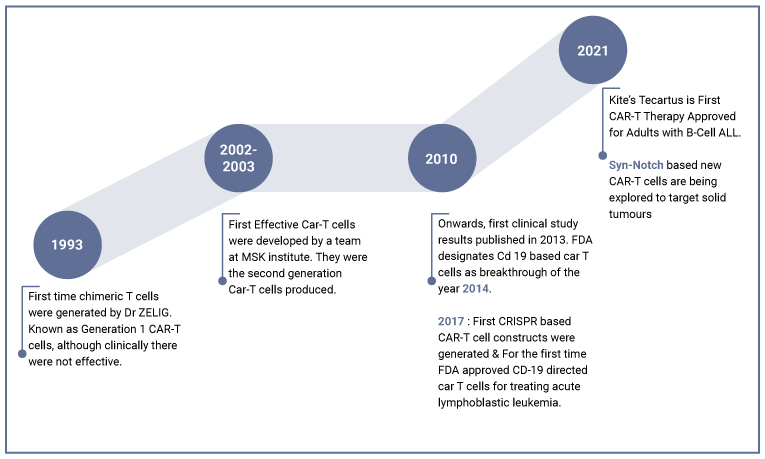
The Chimeric antigen receptor CAR-T cell therapy has revolutionized the immunotherapy field with its high success rate against hematological diseases. Investigations in the early 1980s conceived the idea of tumor-infiltrating lymphocytes; however, reproducibility in invitro hampered further developments. It was not until 1993 Immunologist Dr. Zelig Eshhar created the first generation of chimeric T cells at the Weizmann Institute, Israel. The first generation was successful during experiments, although not clinically effective. Since then, over three decades, a significant chunk of scientific intellect and considerable Research in cancer immunology has optimized this technology further.
Stepping forward to 2021, we have 5 FDA-approved drugs, Diverse manufacturing platforms, and an estimated billion-dollar market, and more than 250 players have invested their portfolios into generating/marketing/manufacturing CAR-T-based therapeutics. Furthermore, now CAR T-based therapies have expanded their horizon into diseases other than oncology, ranging from viral infections such as HIV, and CMV to Autoimmune disorders. Ongoing COVID-19 too finds itself in soup as NCT04324996 sponsored by Chongqing Public Health Medical Centre is currently in phase 2.
However, after decades of modifications, Research & trials, the question remains about its efficacy against solid tumors, and recent advancements, who are the key players developing platforms for next-generation CARs? And the next big breakthrough in this field.
The CARs Generation
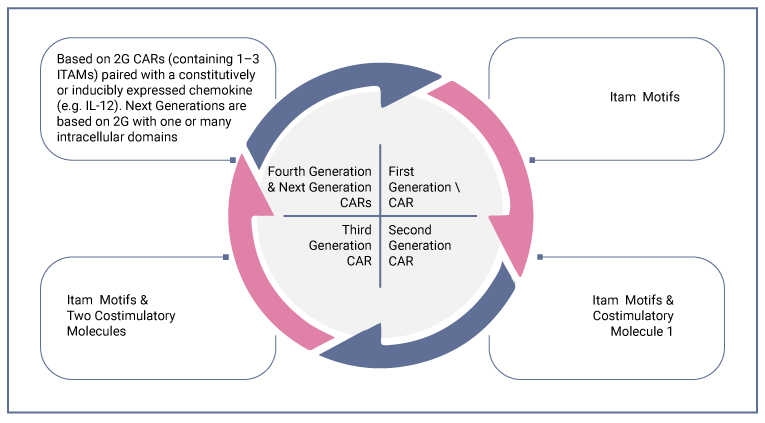
CARs are divided predominantly into three generations; however, incorporating multiple intracellular domains has made them more advanced as the next generation. The division is according to their intracellular signaling domains.
- The first generation: comprises one extracellular domain (scFv) and an intracellular CD3ζ domain.
- Second-generation: CARs have a unique costimulatory part derived from CD28 that significantly improved their clinical efficacy during treatment by increasing the survival of modified T lymphocytes.
- The third generation: consists of molecules having three or more cytosolic costimulatory domains. In addition to CD28, 4-1BB, CD27, ICOS, and OX40 can be coupled which significantly increases the activation, survival, and potency of the genetically engineered T lymphocytes. However, the second-generation CARs have shown the best clinical outcomes and safety to date.
- Next-generation: Consists of One or more intracellular domains.
Status Of Clinical Trials
As of October 2021, about 33 clinical Trials involving CAR-T cells have been completed, 510 in phase 1 out of all the 745 clinical Trials reported so far since the 2000s. Clinical Trials are now focused on targeting other non-oncological diseases.

Challenges, Advancements, and New Frontiers
Faster Wi-Fi means better data transfer which is becoming more and more critical as the quantity and size of data continue to increase along with the higher data demands for flawless communication between multiple integrated devices such as automotive vehicles, connected smart city infrastructure, and so on.
- Solid Tumours: The Syn-notch CAR circuits recently developed at the University of California have demonstrated solid efficacy against solid tumors. Solid tumors remain persistent and are difficult to target with existing CAR-T cell therapies. SynNotch CAR-T cells during experiments have shown superior control of solid tumor burden, demonstrating a better edge over T cells targeting the same antigens compared with mouse models of human mesothelioma and ovarian cancers. Below are the various key players involved in targeting solid tumors.
- HIV: Attempts over-targeting HIV-infected cells expressing gp120 glycoprotein by CAR-T cells (CD 4) successfully destroyed HIV-infected cells. A group led by researchers from the University of California, University of Washington–Fred Hutchinson Cancer Research Center, and CSL-Behring have received federal grants of $13.65 million for this Research.
- Cardiac Fibrosis: Similar attempts have also been conducted in treating cardiac fibrosis by anti-FAP CAR-Ts that have so far been successful in the destruction of affected cardiac fibroblasts. A University of Pennsylvania-based group of researchers recently conducted a study targeting Cardiac fibrosis.
The bottom line is that CAR-T cells are now being tested as multispectral immunotherapy interventions. Boundaries are being expanded gradually, and costs are expected to be cut down with more players in the market.